Socialisation of care: local community as a key player
The healthcare sector is under immense pressure. In May 2018, more than 14,000 Flemish adults with disabilities were waiting on a budget to finance their care. At the same time, Social Services is looking for a solution for 5,000 young people. Flanders now has 80,000 beds in retirement homes: an increase of nearly 25% in the last ten years. You can read these and more figures in this article from De Tijd.
Structural changes are needed to keep up with these trends in the long term. More and more, we should be looking at the socialisation of care as a means to relieve some of that pressure on the public health care sector.
Socialisation of care: what and why?
The socialisation of care might mean a number of things. We define it as following: it is the shift of a non-medical part of our society’s required aid, away from the professional sphere, towards the community.
This community consists of friends and family in the first place, but neighbours too, can play an important role. We consider this contact with the local community to be just as important – for two reasons. Firstly, and quite obviously: neighbours live closeby! They can quickly respond when needed.

In addition, the neighbourhood offers a great potential for expanding the social circle. Not everyone has family or friends (think older, isolated people), but just about everyone has neighbours. Inclusive neighbourhoods can therefore be a great enrichment for people in need of care.
Inclusive neighbourhoods
Care comes in many shapes and forms. Many tasks can just as well be executed by a friendly neighbour, such as:
- pulling up the blinds for an elderly lady
- delivering groceries to people who are less mobile
- helping clear the pavement on snowy days
- offering company against isolation
- occasionally keeping an eye on things
- taking the dog for a walk
- Read how Hoplr neighbours helped each other during the Corona crisis.
Other than that, community service provides some additional benefits.
- If a person in need of care can count on the aid of their family, friends or neighbours, this sometimes means that he or she can keep living in their own home (a little longer). That sense of independence is often important for a person’s well-being.
- If a person in need of care can stay at home for longer, this also relieves some of the pressure on the health care sector. By 2040, 9% of the Flemish population will be over 80. It is therefore important for the healthcare sector that people can live independently for as long as possible by that time.
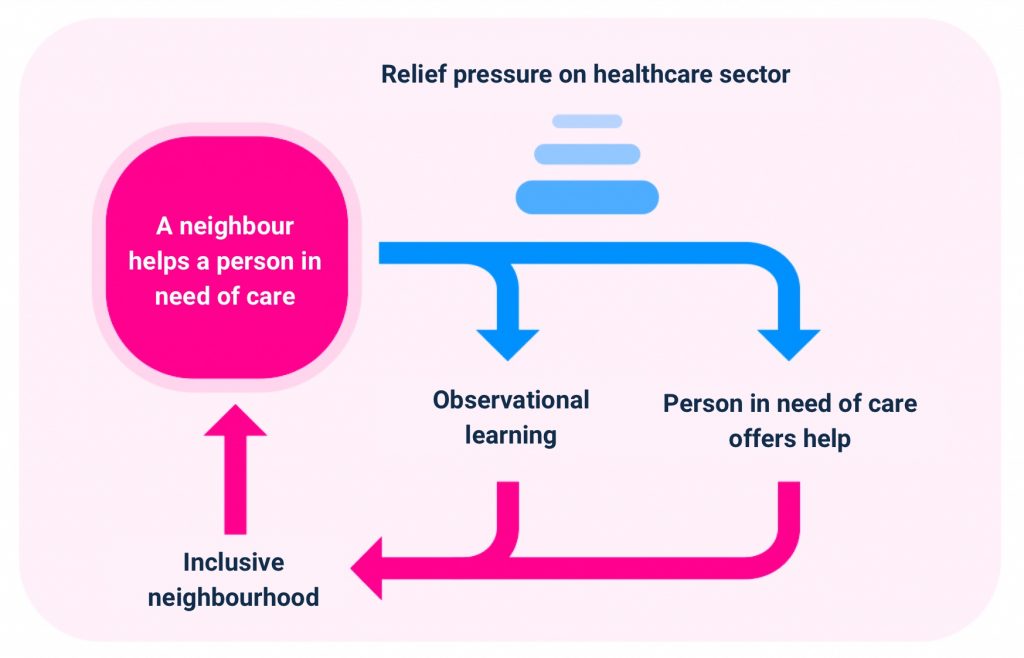
- Any exchange of aid may cause a chain reaction. That effect is called observational learning. You may feel awkward asking a neighbour for help now, but if you see many such exchanges happening around you, the threshold will be much lower.
- Since the care isn’t taking place in a professional sphere, those in need of care can make a contribution themselves. They may no longer be able to carry groceries, but they can perhaps cook a few extra bowls of soup. This way, these people can feel valuable and are less likely to feel marginalised or isolated.
- The community is slowly turning into an inclusive neighbourhood. Asking for help from neighbours is getting easier and the above effects are intensified again.
Pitfall: not all care should be taken on by the community
Despite all benefits, structural socialisation of health care is not something to be taken lightly. It carries some potential dangers.
Two years ago, Belgium introduced a system that allows people with disabilities to spend a predetermined budget on healthcare as desired. As a result, a large healthcare organisation for people with disabilities cut 50 jobs, because the new system couldn’t give them sufficient security.

Similarly, a substantial shift of care towards the community entails a risk of less income security for health care institutions. All the more so, if that informal care involves microtransactions.
Besides that, there’s the danger that socialisation would jeopardise the quality of care. In other words, it is important that non-professional aid is limited to the provision of basic care: shopping, taking a walk together,…
How can Hoplr stimulate inclusive neighbourhoods digitally?
It should be clear that both professional and informal care have an important role within the life of a person in need of care. The model below illustrates the relation between them.
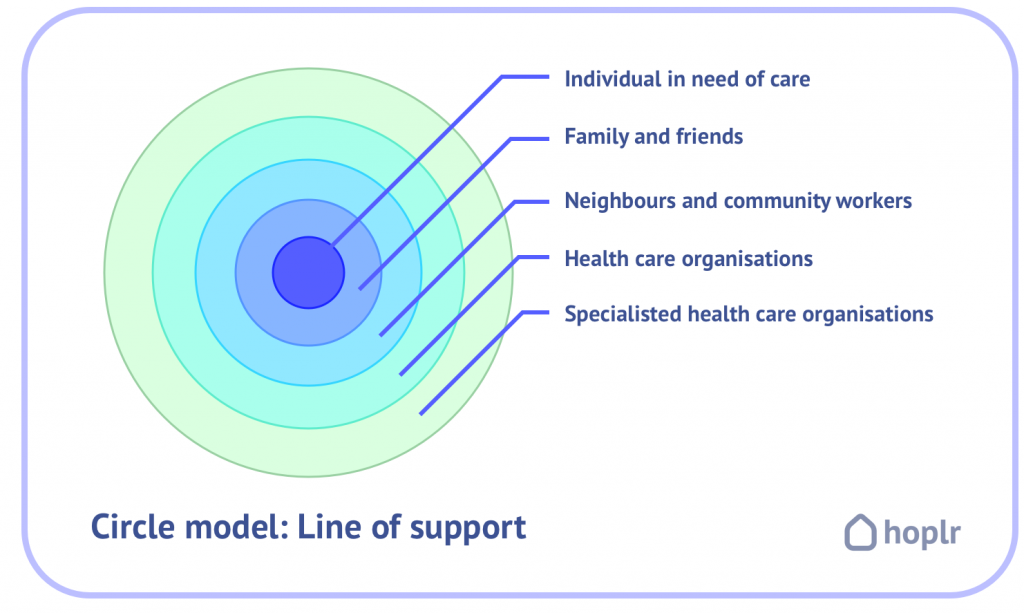
In this model, the community – family, friends, neighbours – serves as first line support. They can easily manage simple requests for help. Only when professional help is required, the appropriate care provider or organisation is called upon. These instances therefore function as a second line support.
Such model is obviously easier drawn up than it is executed, and it will take more than a digital tool alone. Still, we do believe that digital tools can be of great help. Communication is an essential part of structured and fruitful socialisation of care.
First line support

First and foremost, a digital neighbourhood network such as Hoplr allows the person in need of care (or his informal caregiver) to share help requests with the local community. They post their question in the Hoplr neighbourhood or use Hoplr’s neighbour list and private chat to contact specific neighbours.
Conversely, the local community helps keep an eye out. For example, Hoplr users noticed that an elderly neighbour had not brought up her shutters one day and they expressed their concern in the Hoplr neighbourhood. Subsequently, some of them entered her home, saw that she had become unwell and they were able to contact the emergency services in time. An inclusive neighbourhood that is digitally connected, can look out for its own members more easily.
Second line support

Subsequently, a communication line from the neighbourhood to government instances ensures that dependent persons and their informal caregivers can share their questions bottom-up with the appropriate services.
Top-down, governments can stimulate involvement and social cohesion through neighbourhood-oriented communication (information sessions and other events, co-creation, awareness-raising, etc.). The more cohesive the neighborhood, the more its members will look out for one another.
Community workers
Of course, care providers, community workers and local service centres also have a place on Hoplr. By being part of the neighbourhood care network, they can keep in touch with what’s going on more easily, call on the ecosystem of the person in need of care, and capture and answer care questions. They can also keep in touch with the dependent person or their informal caregivers via chat and group chat.
In addition, we must not only take into account the impact on those in need: the socialisation of care also has consequences for citizens who aren’t.
Research shows that neighbours of dependants are more than happy to help, but at the same time they’re not always sure where to go in case of problems they cannot deal with themselves. This can lead to pressure in the neighbourhood. It is therefore essential for them to have a good connection with the appropriate healthcare instances.
Finally, Hoplr stimulates offline encounters. Less anonymity and more connections lead to more involvement and inclusivity. In an inclusive community there is less room for isolation and the most vulnerable members are also taken into account.
Hoplr and the risks of the socialisation of health care
Hoplr offers a positive context for neighbours to get to know each other at their own pace and ultimately to ask for and give help. Everyone needs something at times. Over time, informal care becomes a regular element of the local community.
Hoplr’s help requests are mainly related to chores, doing groceries and social contact – much less in the sphere of medical or professional care. Additionally: care via Hoplr is always voluntary.
Social value
Our society faces a number of challenges, including the increasing pressure on the healthcare sector. By connecting, engaging and mobilising people, we aim to contribute to inclusive neighborhoods and thus, a more inclusive society.







